How To Differentiate An Angina Pectoris From A Heart Attack?
Angina pectoris and myocardial infarction are two conditions that fall within the category of ischemic heart disease. The latter refer to a cardiac injury that occurs when the blood flow to the heart is disturbed.
The problem is that both situations produce similar symptoms and they tend to be confused. In addition, its incidence has risen considerably in recent years, especially due to the modern lifestyle.
Today, acute myocardial infarction remains a major cause of death. Angina pectoris is considered a major risk factor for heart attack. Therefore, this time we explain how they differ and how they are treated.
What is angina pectoris?
Angina pectoris occurs when blood flow to the vessels that supply the heart is temporarily reduced. They are the so-called coronary arteries, which are responsible for nourishing the myocardium, which is the muscle that allows the heart to beat and pump blood.
When the muscle does not receive enough oxygenated blood, the heart cannot function properly. Unfortunately, these arteries are very susceptible to atherosclerosis, as they are small in size.
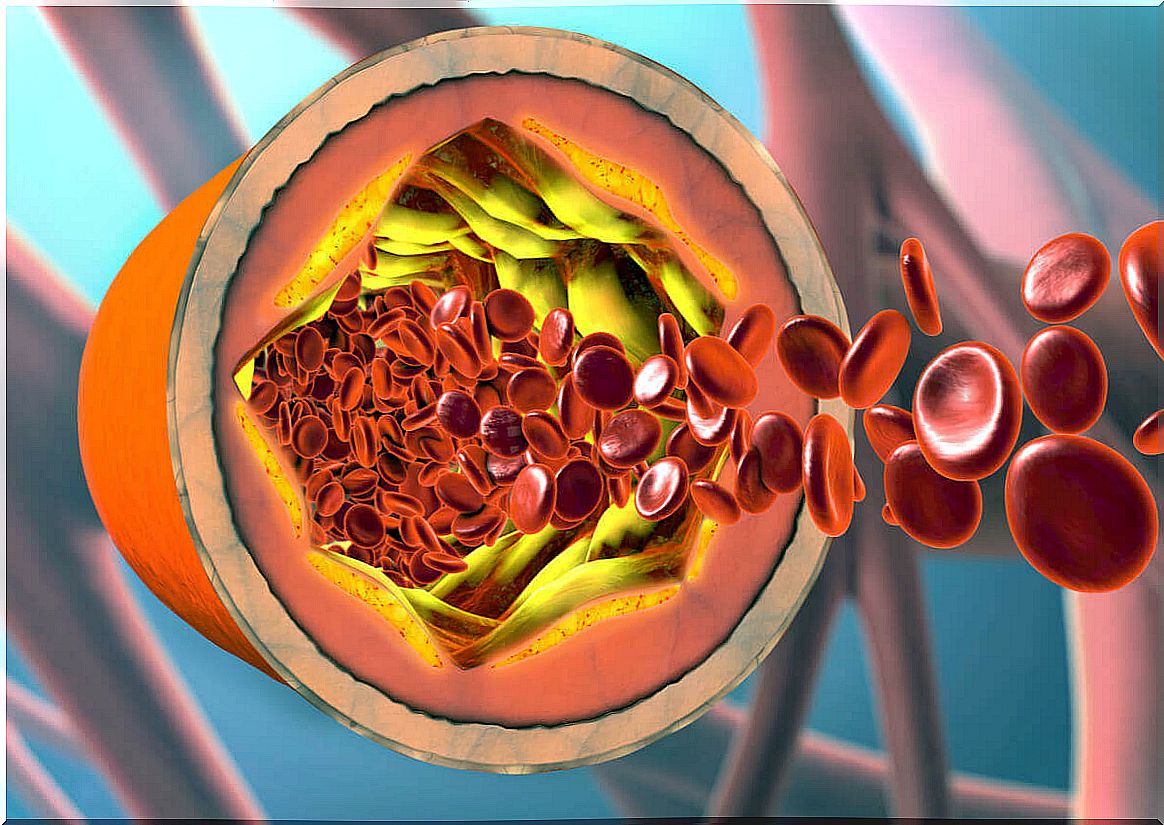
The development of atherosclerosis occurs when fatty deposits accumulate in the blood vessels, causing a narrowing. In angina pectoris, this obstruction makes it difficult to nourish the heart muscle in situations where more oxygen is needed, as blood flow becomes insufficient.
However, it can also cause problems in situations of cold, stress or in patients who smoke, as it causes the coronary arteries to contract and narrow.
What is a myocardial infarction?
Myocardial infarction is a sudden blockage of blood flow to the heart. Its cause, as in angina pectoris, is usually atherosclerosis. However, in this particular case, the fatty plaque present in the arteries breaks down.
As a consequence, a clot is formed that obstructs some of the coronary arteries and, in turn, a situation of ischemia occurs. The latter is when the myocardium runs out of oxygen and its cells die.
Many doctors consider angina pectoris a warning situation for the heart attack itself. Angina does not cause definitive damage to the heart, but heart attack does, and both situations are usually preceded by a blockage in the coronary arteries.
What is the difference between angina pectoris and heart attack?
Undoubtedly, the main difference between these pathologies is that a heart attack causes an injury to the heart, while angina does not. But, in addition to this, there are other differences at the symptomatic level that allow guiding the diagnosis.
The heart attack produces a very intense pain in the center of the chest that usually radiates towards the left arm. In some situations, depending on where the muscle damage has occurred, the pain can spread to the right arm.
This pain does not go away or get better with nitroglycerin, a drug that helps the arteries dilate. In the case of angina, when nitroglycerin is administered, it does usually reduce pain.
In addition, the heart attack is usually accompanied by shortness of breath and profuse sweating. In angina pectoris, the pain is not as severe and does not radiate. There is also no dyspnea, and symptoms can go away on their own in most cases.

Are there other differences?
In addition to the symptomatic differences that we have mentioned, there are other important aspects that must be taken into account. In angina pectoris, sometimes the reason that triggered the episode can be found.
For example, when pain appears after physical exercise or strong emotions, it is indicative of angina. However, it is convenient to bear in mind that, even if the symptoms remit, it is necessary to consult a doctor and treat the situation.
That leads us to another difference: treatment. Adopting healthy habits to reduce or stop atherosclerosis may be enough to treat some cases of angina pectoris. Nitrates, blood-thinning drugs, and cholesterol-lowering drugs are also used.
However, it is true that in many cases an intervention is required to ensure that the coronary arteries have adequate flow. In the case of heart attack, it is essential to reestablish blood flow, so treatment usually includes coronary intervention.
Angina pectoris and heart attack deserve attention
Both conditions are serious and life threatening. Any symptoms we have mentioned should be treated as a medical emergency. It should be the cardiology professional who carries out the pertinent studies to find out what pathology it is.